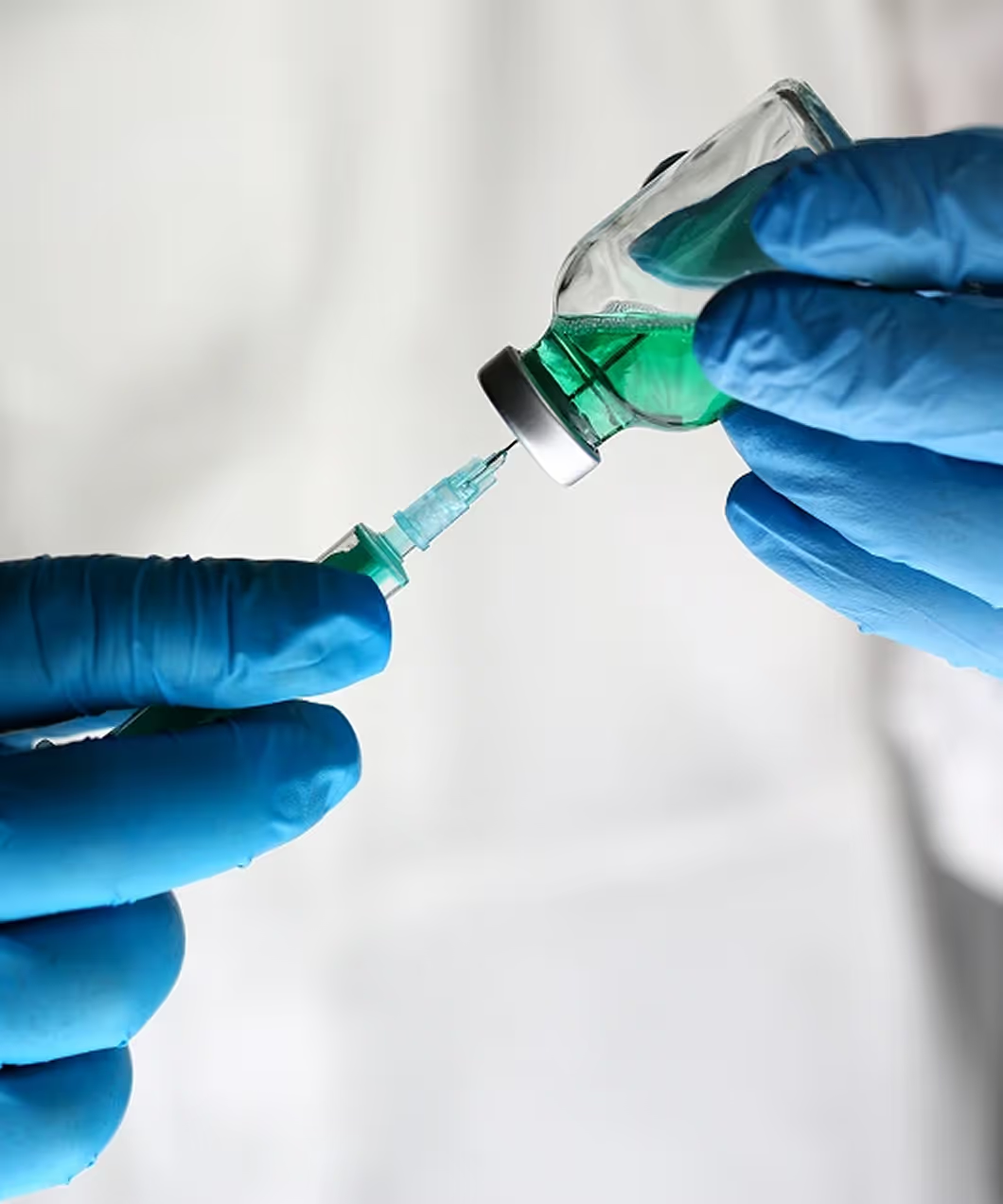
Microsurgical
Varicocele Repair
Struggling with dull testicular pain, shrinking testes, low sperm count, or dipping testosterone from varicoceles, the hidden culprit in up to 45% of male infertility cases? The Y Factor's Dr. Russel Williams, with 25 years of microsurgery expertise, performs the 30-minute outpatient subinguinal varicocelectomy — a minimally invasive procedure that clips dilated veins under magnification, boosts sperm production, halts atrophy, and revives natural hormone levels with just a tiny, suture-free incision and minimal downtime.
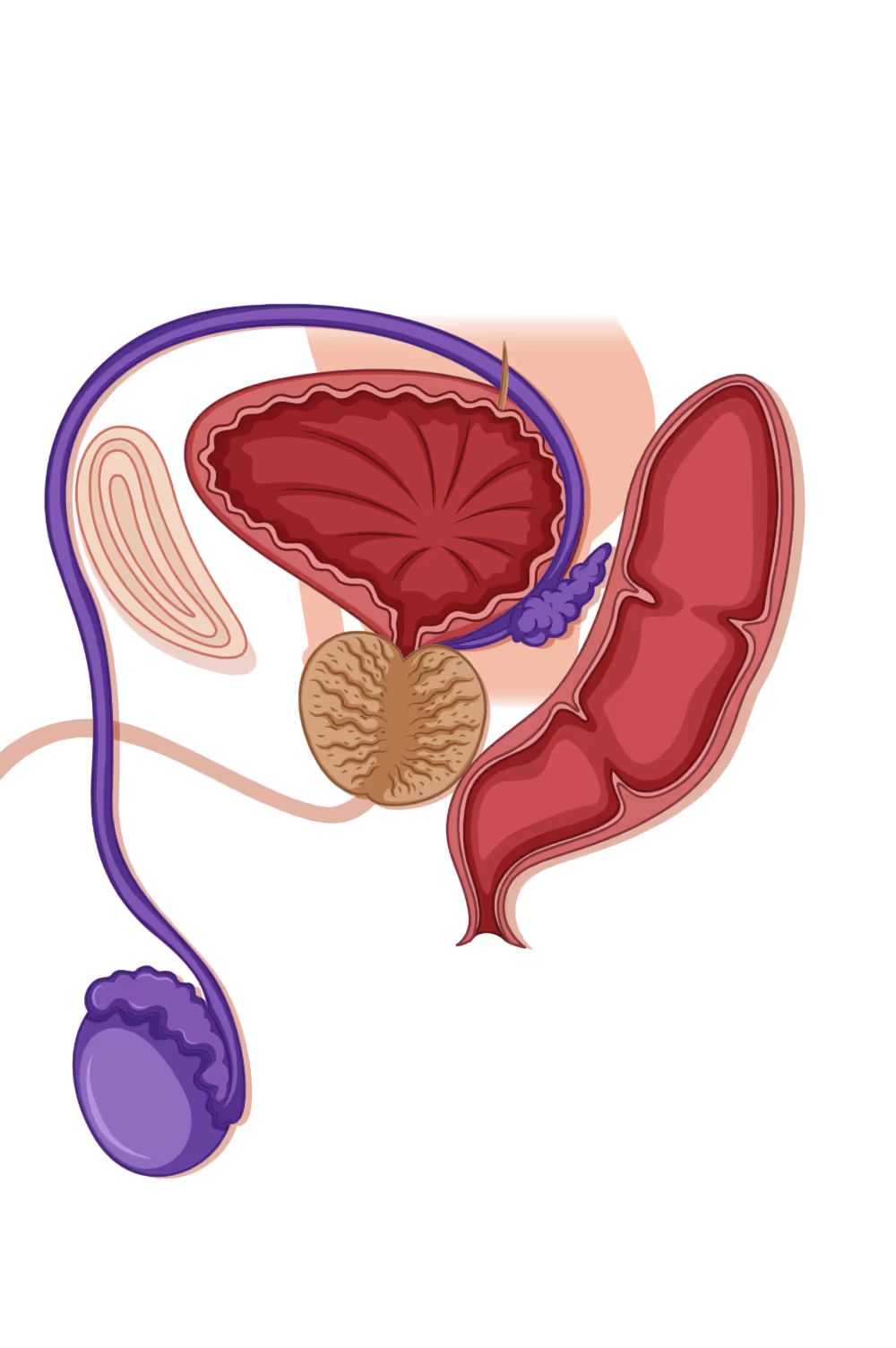

Varicocele Treatment in Houston
Men seeking effective varicocele treatment in Houston often face a confusing array of options. Varicoceles are not merely "varicose veins" in the scrotum. They are a progressive medical condition that damages testicular function through heat stress and oxidative damage.
At The Y Factor, we specialize in the microsurgical subinguinal varicocelectomy, treating the root cause of your symptoms rather than just managing them.

The Gold Standard for Male Fertility and Testosterone Optimization
Varicoceles serve as a primary root cause for both male infertility and low testosterone. The condition causes an abnormal accumulation of blood, raising the scrotal temperature. This heat stress suppresses natural hormone production and degrades sperm quality over time.
The 2024 AUA/ASRM Guidelines confirm that microsurgical repair is the preferred technique for preserving testicular function and improving fertility outcomes. An experienced physician will perform this 30-minute outpatient procedure to target the underlying dysfunction directly.

Why Microsurgical Varicocelectomy Outperforms Embolization
Patients often compare surgical repair with radiological embolization options. While providers may market embolization as a "convenient" nonsurgical alternative, clinical data favors microsurgery for long-term success. The microsurgical approach offers distinct advantages for men who prioritize results:
- Lower recurrence rates: Microsurgical repair consistently demonstrates recurrence rates of approximately 1% compared to embolization rates that can reach 10%–15% in some series.
- Superior fertility outcomes: Recent comparative studies have shown that microsurgery yields significant improvements in sperm parameters compared to catheter-based blocking techniques.
- Precision technique: The microsurgical approach allows the surgeon to visualize and preserve testicular arteries and lymphatics. This prevents complications like hydrocele while ensuring every problematic vein is ligated.
How Varicocelectomy Works

Techniques Used in Varicocele Repair
Several surgical approaches exist, including microsurgical and minimally invasive techniques. The specific approach depends on anatomy, clinical findings, and surgeon expertise.
Regardless of technique, careful identification of structures is essential to minimize complications.

Signs You Need a Varicocele Specialist in Houston, Texas
Generic urology checkups often miss the subtle signs of testicular stress. You need a dedicated varicocele specialist in Houston, Texas, if you experience specific warning signs that suggest underlying vascular issues:
- Infertility: You have struggled to conceive for six to 12 months despite having a partner with normal fertility.
- Physical discomfort: You notice a dull ache or "dragging" sensation in the scrotum that worsens after standing or exercise. This is sometimes described as feeling like a "bag of worms."
- Hormonal decline: You experience symptoms of low testosterone, such as fatigue or brain fog, alongside testicular changes.
We use advanced Doppler ultrasound to detect even "subclinical" varicoceles that standard physical exams miss. A proper diagnosis helps you understand why previous treatments may have failed.
%202.avif)
Restoring Your Biology: Impact on Sperm and Testosterone
Repairing a varicocele acts as a biological "reset" for your testicles. The procedure removes the oxidative stress and heat that damage your DNA and suppress hormone output:
- Boost testosterone: Research published in 2024 confirms that microsurgical varicocelectomy results in statistically significant increases in serum testosterone levels for subfertile men.
- Repair DNA: A 2025 study highlights that varicocelectomy significantly reduces sperm DNA fragmentation. This addresses a key infertility factor that embolization handles less effectively.
- Prevent decline: Evidence from a 2025 study supports early intervention to prevent progressive damage to testicular function. The data suggests that waiting often leads to further degradation of sperm quality.
Risks and Recovery
Risks of varicocelectomy include:
- bleeding
- infection
- hydrocele formation
- recurrence
Recovery typically involves:
- limited activity initially
- gradual return to normal activity
- follow-up semen analysis over time
Most men recover without significant issues.
Varicocelectomy and Fertility Planning
Varicocelectomy is often one component of a broader fertility plan that may include:
- hormonal evaluation
- lifestyle optimization
- assisted reproductive strategies when appropriate
Timing and expectations are coordinated carefully.
.avif)
What to Expect: Procedure, Recovery and Varicocele Surgery Cost
We prioritize efficiency and transparency for every patient. Your journey begins with a same-day consultation and an on-site Fertility Evaluation to assess your needs.
- Efficient care: Our specialists perform the procedure in just 30 minutes using light sedation, allowing you to return home the same day.
- Rapid recovery: Most men return to light activities within 48 hours. The tiny incision is often hidden in the natural groin crease.
- Transparent pricing: We accept major insurance plans and provide clear "no surprise" pricing for self-pay patients regarding varicocele surgery cost.
Schedule Your Evaluation With The Y Factor
Do not wait while your fertility or testosterone levels decline. A semen analysis and ultrasound can confirm if a varicocele is limiting your health. Contact The Y Factor today to address the root cause with microsurgical varicocele surgery and restore your potential.
.svg)