Enlarged Prostate (Benign Prostatic Hyperplasia)
Benign prostatic hyperplasia (BPH), commonly referred to as an enlarged prostate, is one of the most common urologic conditions affecting men as they age. Despite its prevalence, BPH is frequently underrecognized or dismissed as a normal part of aging—leading many men to tolerate bothersome urinary symptoms for years before seeking care.
At The Y Factor, enlarged prostate symptoms are evaluated through a diagnostic-first, physiology-driven approach. Rather than assuming symptoms are inevitable or immediately pushing intervention, we focus on understanding how prostate size, bladder function, and urinary dynamics interact so that care decisions are informed, appropriate, and aligned with each patient’s long-term health and quality of life.

What Is an Enlarged Prostate?
The prostate is a walnut-sized gland located just below the bladder and surrounding the urethra. Its primary function is to produce seminal fluid. As men age, prostate tissue commonly enlarges due to hormonal and cellular changes. When this enlargement begins to interfere with urine flow, it is referred to as benign prostatic hyperplasia.
“Benign” means non-cancerous. BPH is not prostate cancer, but its symptoms can significantly affect daily functioning, sleep, and overall well-being.

What Causes Benign Prostatic Hyperplasia (BPH)?
BPH develops gradually over time and is influenced by multiple factors, including:
- age-related hormonal changes
- lifelong exposure to testosterone and its metabolites
- changes in prostate cell growth and turnover
- metabolic health and inflammation
While nearly all men experience some degree of prostate growth with age, not all men develop symptoms. The degree to which enlargement affects urinary function depends on prostate anatomy, bladder health, and individual physiology.

How an Enlarged Prostate Affects Urination
Because the prostate surrounds the urethra, enlargement can compress or narrow the urinary channel. This may lead to:
- resistance to urine flow
- incomplete bladder emptying
- increased bladder pressure and muscle strain
Over time, the bladder may become overworked, leading to urgency, frequency, or reduced bladder capacity—even if prostate enlargement itself is modest.

Common Symptoms of an Enlarged Prostate
Symptoms of BPH are often grouped under lower urinary tract symptoms (LUTS) and may include:
- weak or slow urinary stream
- difficulty starting urination
- stopping and starting during urination
- frequent urination
- urgency
- waking at night to urinate
- sensation of incomplete bladder emptying
Symptoms may progress gradually and vary in severity from day to day.
BPH vs Other Causes of Urinary Symptoms
Not all urinary symptoms are caused by prostate enlargement. Similar symptoms may arise from:
- bladder overactivity
- neurologic conditions
- urinary tract irritation or infection
- medication effects
This overlap makes diagnostic evaluation essential. Treating symptoms without identifying the underlying cause may lead to incomplete relief or worsening bladder function over time.
Why BPH Is Often Underdiagnosed or Delayed
BPH is frequently delayed or underdiagnosed because:
- symptoms are assumed to be normal aging
- men adapt behaviors (fluid restriction, bathroom planning)
- symptoms develop slowly
- embarrassment prevents discussion
Unfortunately, untreated BPH may place increasing strain on the bladder and urinary system.
How Enlarged Prostate (BPH) Is Evaluated
Clinical History and Symptom Scoring
Evaluation begins with a detailed discussion of urinary symptoms, including:
- frequency and timing
- nighttime symptoms
- severity and progression
- impact on sleep and quality of life
Symptom scoring tools may be used to quantify severity and track changes over time.
PSA Testing and Laboratory Evaluation
Prostate-specific antigen (PSA) testing may be included as part of the evaluation. PSA levels help provide context but must be interpreted carefully, as PSA can be influenced by many factors beyond prostate size alone.
Testing decisions are individualized based on age, symptoms, and risk factors.
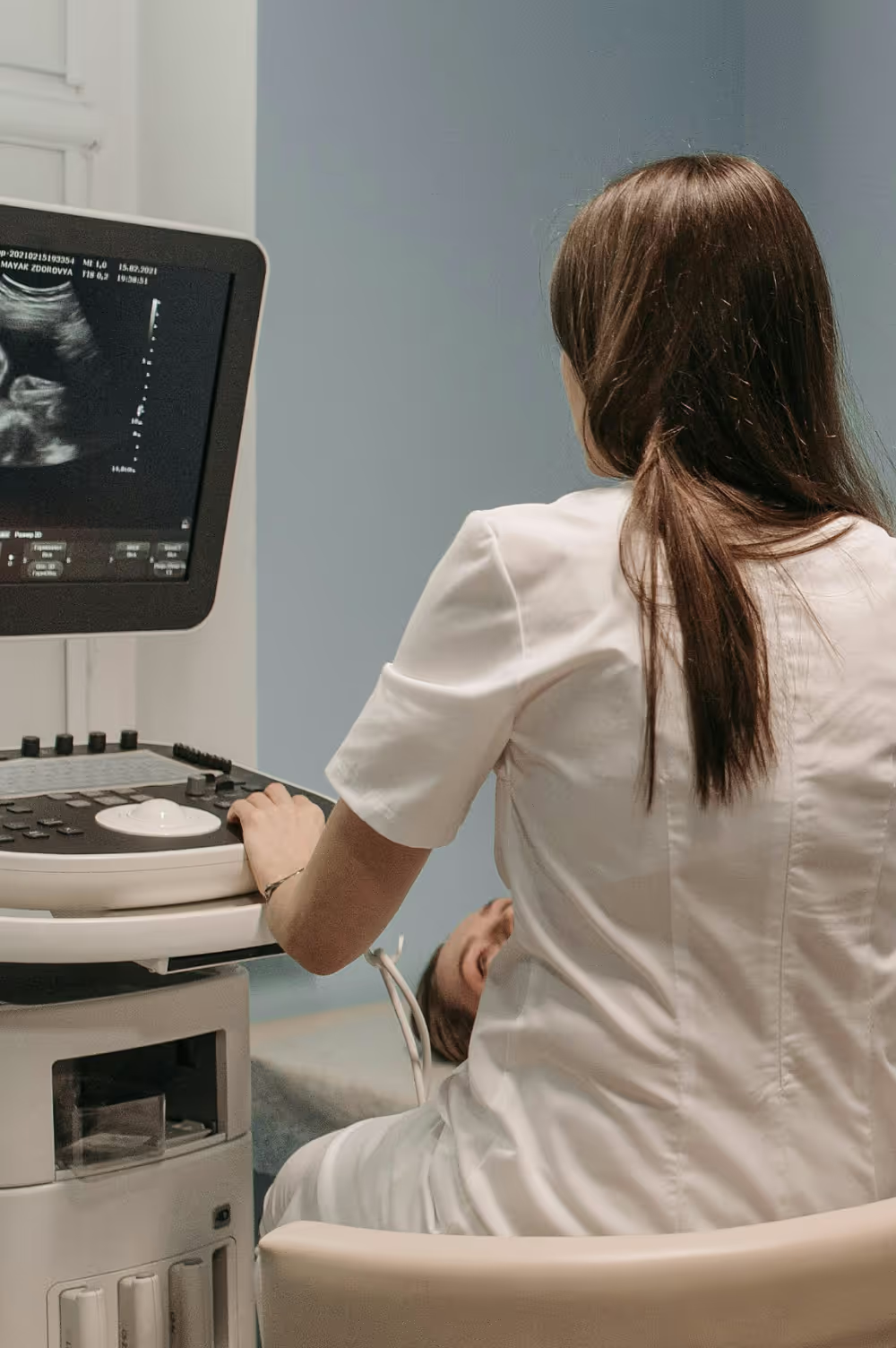
Ultrasound and Bladder Testing
Ultrasound imaging plays a critical role in BPH evaluation. Imaging may assess:
- prostate size and anatomy
- bladder wall characteristics
- post-void residual urine volume
Post-void residual testing helps determine whether the bladder is fully emptying or retaining urine due to obstruction or dysfunction.
BPH, Bladder Health, and Long-Term Risks
If left untreated, BPH may contribute to:
- progressive bladder dysfunction
- worsening urgency and frequency
- recurrent urinary retention
- reduced quality of life
Early evaluation allows for monitoring and intervention before irreversible bladder changes occur.
.avif)
When Men Should Seek Evaluation for BPH
Men should consider evaluation if they experience:
- persistent urinary symptoms
- worsening stream or incomplete emptying
- frequent nighttime urination
- urinary symptoms affecting daily activities or sleep
Early assessment provides clarity and reassurance.
Schedule an Enlarged Prostate Evaluation
The Y Factor provides comprehensive enlarged prostate (BPH) evaluation in Houston, integrating diagnostic imaging and clinical oversight to identify the cause of urinary symptoms and guide individualized care planning.
.svg)