Pelvic and Scrotal Pain in Men
Pelvic and scrotal pain is a common yet highly complex urologic complaint in men. Pain may involve the testicles, scrotum, perineum, lower abdomen, or deep pelvic structures, and it may present as sharp, dull, aching, or intermittent discomfort. For many men, these symptoms are frustrating, anxiety-provoking, and difficult to describe—leading to delays in diagnosis and care.
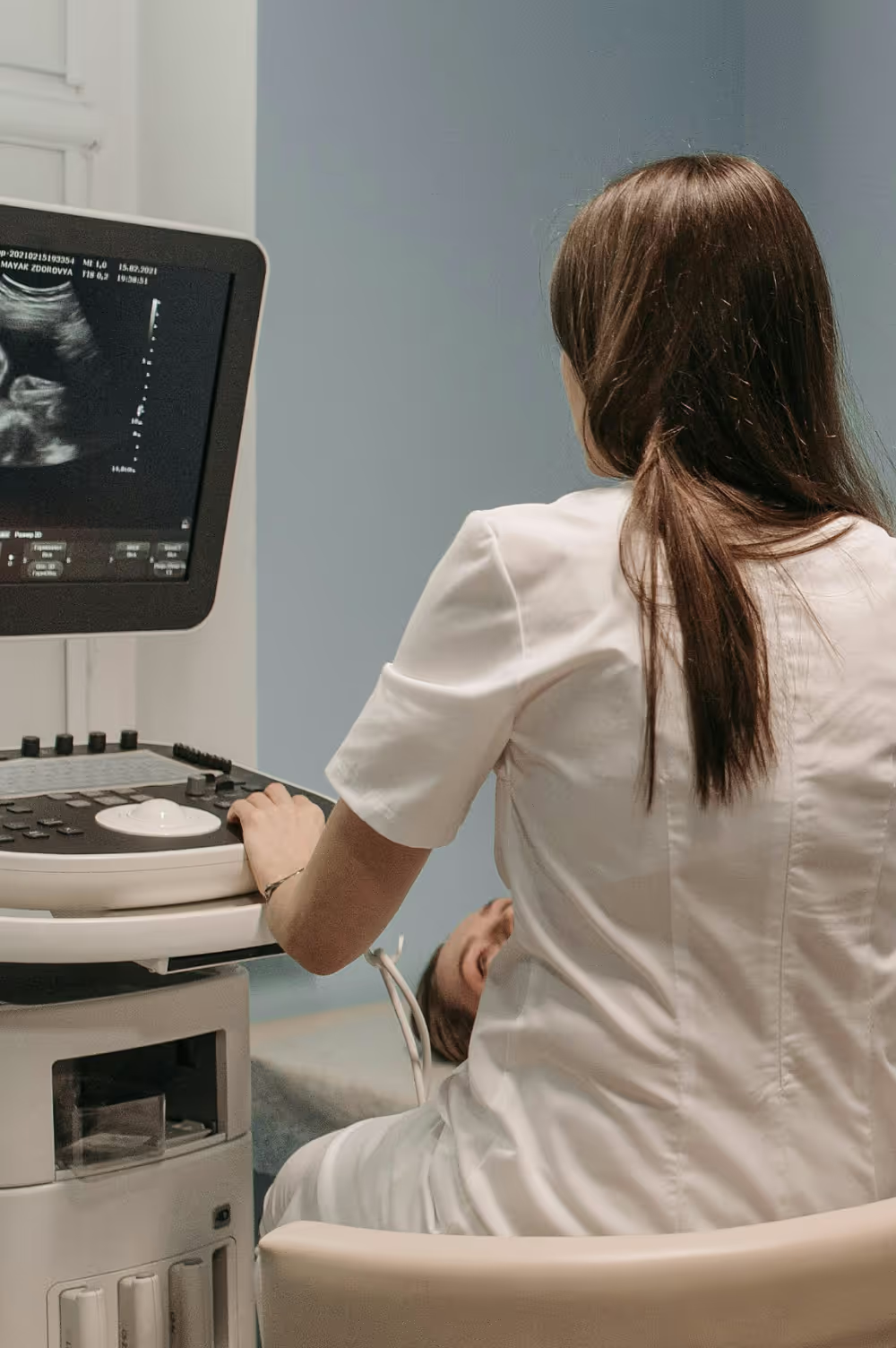
At The Y Factor, pelvic and scrotal pain is approached through a diagnostic-first, systems-based framework. Rather than assuming pain is purely infectious or dismissing symptoms as “non-specific,” we focus on identifying the underlying anatomic, vascular, neurologic, or inflammatory contributors so that care is targeted and effective.
.webp)
What Is Pelvic and Scrotal Pain?
Pelvic and scrotal pain refers to discomfort localized to:
- the scrotum or testicles
- the perineum (area between the scrotum and anus)
- the lower pelvis or groin
- surrounding structures that refer pain into this region
Pain may be constant or episodic, mild or severe, and may worsen with activity, sitting, ejaculation, or urination.
Importantly, pelvic and scrotal pain is a symptom, not a diagnosis. Identifying the cause requires careful evaluation.

Why Pelvic and Scrotal Pain Is Complex
The pelvis contains overlapping systems:
- urologic structures
- nerves and muscles
- blood vessels
- reproductive organs
Pain originating in one area may be felt elsewhere, making localization difficult. In addition, pelvic pain often involves multiple contributors rather than a single cause, particularly when symptoms persist over time.
Common Causes of Pelvic and Scrotal Pain
Inflammatory and Infectious Causes
Inflammation of the epididymis, testicle, or surrounding tissues can cause scrotal pain and tenderness. While infections are an important consideration, not all inflammatory pain is infectious in nature.
Symptoms may include swelling, warmth, or discomfort that worsens with activity or touch.
Musculoskeletal and Nerve-Related Pain
Pelvic floor muscle dysfunction, nerve irritation, or referred musculoskeletal pain may cause chronic pelvic or scrotal discomfort. This type of pain is often:
- positional
- worsened by sitting
- variable in intensity
Neuropathic pain may feel burning, sharp, or radiating.
Vascular Causes (Including Varicocele)
Varicoceles—enlarged veins within the scrotum—are a common cause of dull, aching scrotal pain, particularly with prolonged standing or physical exertion. Vascular congestion may worsen throughout the day and improve when lying down.
Vascular causes are often underdiagnosed without imaging.
Referred Pain from the Prostate or Bladder
Conditions affecting the prostate or bladder may refer pain into the pelvis or scrotum. Prostate inflammation, bladder dysfunction, or pelvic nerve irritation can all present as scrotal or perineal discomfort.

Acute vs Chronic Pelvic and Scrotal Pain
Acute pain develops suddenly and may require urgent evaluation, particularly if accompanied by swelling, redness, or systemic symptoms.
Chronic pelvic or scrotal pain persists for weeks or months and often involves overlapping contributors. Chronic pain requires a thoughtful, stepwise diagnostic approach rather than repeated empiric treatment.

Symptoms Men Should Not Ignore
Men should seek evaluation for:
- persistent or worsening scrotal pain
- unilateral swelling or asymmetry
- pain associated with fever or systemic symptoms
- discomfort affecting sexual activity or fertility
- pain that interferes with daily life
Early evaluation reduces anxiety and prevents unnecessary progression.

Why Pelvic and Scrotal Pain Is Often Misdiagnosed
Pelvic and scrotal pain is frequently misdiagnosed because:
- symptoms are non-specific
- pain may fluctuate
- imaging is not performed
- focus is placed solely on infection
Without a comprehensive evaluation, underlying vascular or structural causes may be missed.
How Pelvic and Scrotal Pain Is Evaluated
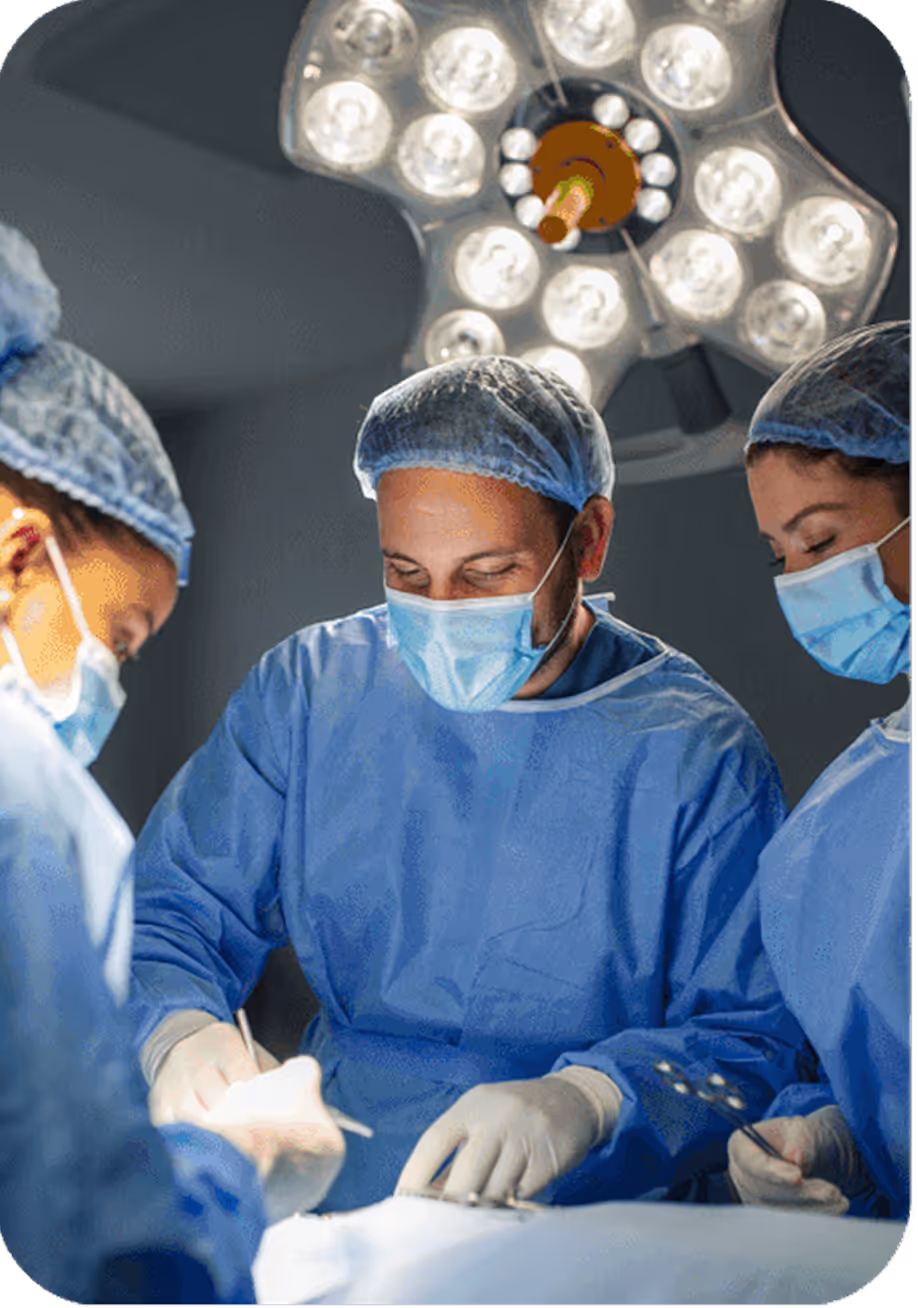
Clinical History and Physical Examination
Evaluation begins with a detailed history, including:
- onset and duration of pain
- aggravating and relieving factors
- associated urinary or sexual symptoms
- prior infections, trauma, or procedures
A focused physical exam helps identify tenderness, swelling, or structural abnormalities.
Know More
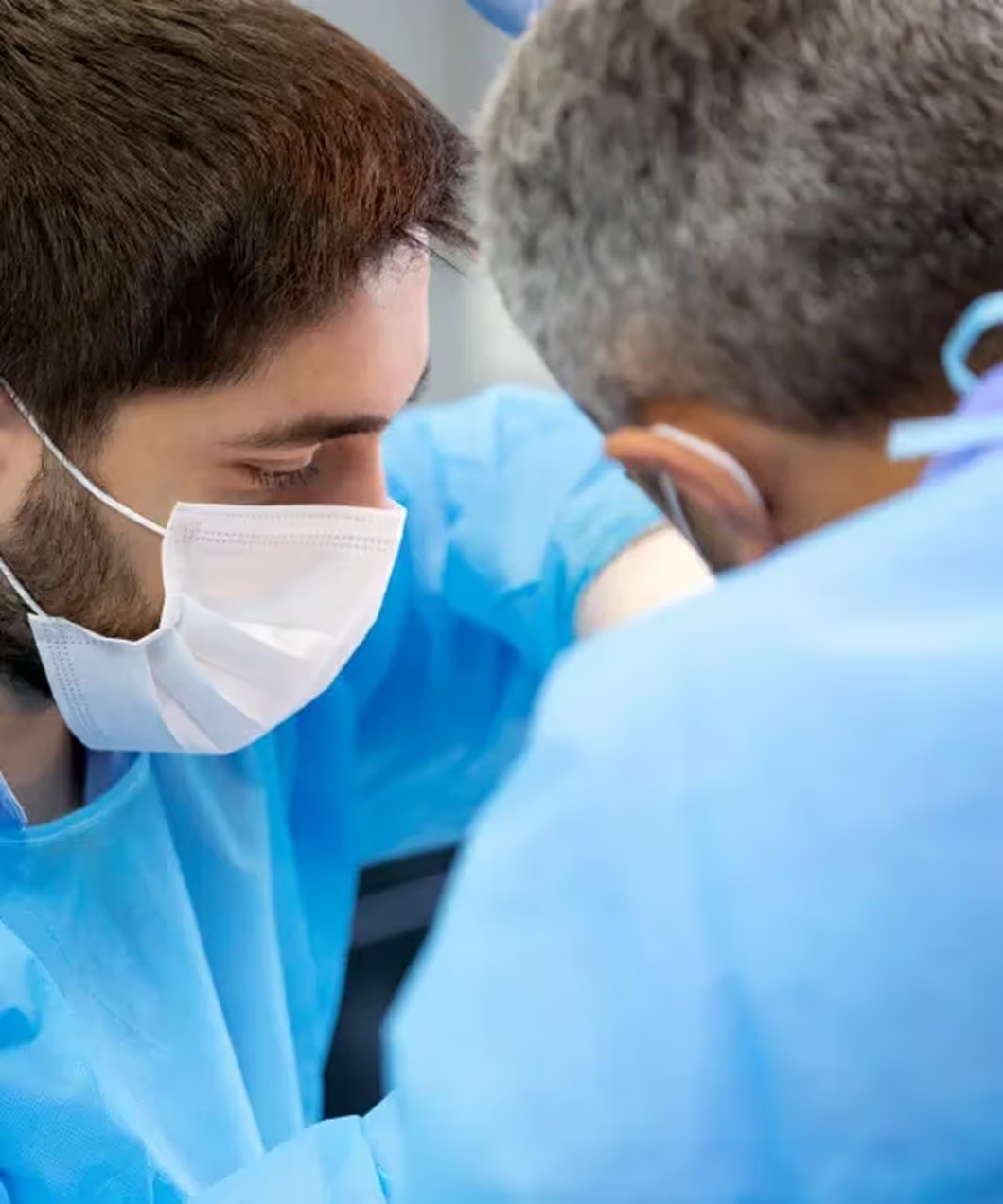
Pelvic and Scrotal Pain, Sexual Function, and Fertility
Pain in the pelvis or scrotum may affect:
- sexual comfort
- erectile function
- ejaculation
- sperm production
An integrated evaluation ensures that pain management aligns with sexual and reproductive health goals.
.avif)
When Men Should Seek Evaluation
Men should consider evaluation if they experience:
- ongoing or recurrent pelvic or scrotal pain
- pain affecting quality of life
- discomfort with no clear explanation
- symptoms related to fertility concerns
Timely evaluation allows for accurate diagnosis and individualized care planning.
Schedule a Pelvic or Scrotal Pain Evaluation
The Y Factor provides comprehensive pelvic and scrotal pain evaluation in Houston, integrating diagnostic imaging and clinical oversight to identify the underlying cause of pain and guide appropriate care.
.svg)